Subvisible Thoughts: Rewriting the War on Microbes
The auditorium was dark and air-conditioned. As lectures on yeast, HIV, and tuberculosis floated over my head, I scribbled notes in three languages: original Portuguese, translated English, and vocabulary I made up to lasso my thoughts onto paper. Words like subvisible, macrobe, germophile, biofiction and endogarden squeezed in sideways next to sketches of virions and DNA on the pages of my Watson journal.
Do you have that one study trick when you want to get ideas flowing? Maybe you need perfect silence of the library quiet room, or Frank Ocean in your earbuds. Simón Bolívar claimed to do his best thinking at the center of a crowded ballroom. Turns out, the overly-chilled halls of an infectious disease conference were my ideal habitat for incubating ideas.
As a species, human beings are extremely visual. Our eyes let us see a rainbow of colors, pick out meaning from black squiggles on a screen, and react to danger (like that of a snake across our path) before our mind consciously registers the threat. As eyes evolved, our smell, taste, touch, and hearing dwindled to perfunctory senses. Compare our nose to a dog’s, our ears to a bat’s, our tongue to a snake’s, or our touch to that of a star-nosed mole.
Our sight makes us biased. We save colorful species from extinction, yet we wonder if little brown birds can be that important to an ecosystem. We photograph wildflowers and ignore bark, stems, and roots. We cuddle stuffed jaguars and lions, but when was the last time you snuggled a plush microbe? (They do exist!)
Our excellent eyesight is limited by scale. We can’t see anything narrower than 0.04 millimeters. At least, we can't distinguish an object smaller than 0.04 millimeters from its neighbor. When we see a conglomeration of tiny particles, like the atoms in a table or the mold cells in a colony, we see their cumulative mass, not their individual bodies. Our eyesight's resolution probably isn't going to get much better, because it's already approaching its quantum limit.
What would our relationship to microbes be like if we were a primarily smelling or tasting organism? Might we know salmonella and leptospira like we do jaguars and lions? Might we develop compassion and curiosity for pathogens, despite their ability to harm us? After all, we find a place in our hearts for macrobes that threaten the same: wolves, pumas, bears, and on down the list of beloved predators.
And that brings me to my next idea.
Artists and writers bring to life what our limited senses cannot. Impressionists paint motion and light into landscape. Surrealists depict the unconscious world of dreams. Poets tempt the sixth mass extinction into tangible proximity. (Check out The After, a poem about Anthropocene extinction by Melinda Mueller, my high-school biology teacher.)
One of the first things I learned in my favorite college course, Don Snow's “The Nature Essay,” was to write sensually. Breathe in Ellen Meloy's juniper scent, feel Amy Irvine's canyon mud suck your feet down, taste durian through David Quammen's prose. These nature writers push beyond vision to awaken worlds for their readers.
Could we write microbes sensually? The genre might be called “speculative biofiction.” I want someone to evoke the satin skin of a gram-negative bacterium, the rigid reluctance of a gram-positive. I want to imagine the sour tang of Yersinia or the sweet tickle of Plasmodium on the tongue. (No sampling pathogens, please!) I want to attend a party of Lactobacillus through scent, following their appetites as they converge on a silo of sprouted barley and nibble in into beer.
I want someone to describe the barbed armor and biochemical antics of two Streptococcus colonies as they battle for control of a Petri dish, so I can root for my favorite without having to peer down the eyepiece of an elusive microscope. I want to swim through the bloodstream and slip into DNA with an HIV virion. Could we transition from a society of germaphobes to one of germophiles?
I don’t have a microscope, and neither does anyone else outside a handful of college students and microbiologists. Scopes give me a headache, anyway. Let’s write microbes sensually, so we can cultivate compassion and curiosity for these remarkable little ones.
By now you might be asking… why does it matter if we have compassion and curiosity for microbes?
Perhaps obviously, infectious disease is defined as an illness arising from an infectious agent: a pathogen, a germ, a microbe. This week, as I sat through dozens of presentations on infectious disease, I expected to see quite a few microbes on the projector screen.
Total microbe count: one.
Chikungunya was paired with images of swollen ankles, tuberculosis with scatter plots, candida with symptom charts. I knew I wouldn’t get to smell, taste, or feel microbes at a professional conference, but damn, I barely got to see a picture!
“Aedes aegypti mosquito vector eradicated in Brazil! Accidentally reintroduced twice…”
“Antibiotic kills Mycobacterium tuberculosis! Now, multi-resistant Tb is more lethal than ever…”
“Yellow fever was conquered for good! Now it's reemerging as climate shifts the habitat of its wildlife host, Amazonian monkeys….”
The story of disease I heard at the DIERN conference tells that humans are engaged in warfare with microbes. We grasp onto this narrative because it's familiar. We have been waging war on macro-predators for millennia, and we've been winning. Saber-toothed lions went extinct; gray wolves and Bengal tigers are confined, for the most park, to controlled populations in parks. Although predators still take lives (read about human-wildlife conflict in Nepal, California, or Brazil), their impact on the human species is a shadow of what it once was.
But I think this narrative of war makes less sense when we look at our relationship with microbes. Our campaigns against large predators worked because we share a scale. Our smaller foes, the microbes, will not be so easy to knock off. If we declare war, we may be setting ourselves up to lose.
Microbes operate on their own scale. Bacteria are generally about one micron wide. That's a millionth of a meter, six orders of magnitude smaller than you or me. Protozoan parasites are slightly larger, hovering around 50 microns. Don't even get me started on viruses. Those tiny machines are measured in nanometers. That's one billionth of a meter, or nine orders of magnitude smaller than us! If we are engaged in a war, then scale is the microbes' deadliest weapon, because it gives them two superpowers: speed and stealth.
Speed, in terms of evolution. Microorganisms evolve faster than you can load a YouTube video on sketchy WiFi. The typical generation time of E. coli is 20 minutes. The average for a human is about 15,000,000 minutes. Shorter generations allow faster evolution. E. coli and their ilk have us beat with their hands (ahem, flagella) tied.
Stealth, in terms of hiding from us. Tiny things are not only hard to see with our eyes, they are also hard to detect and target with our weapons, like medicines and immune systems. They evade our weapons by evolving around them. In the last eight years, Enterobacteria have started producing an enzyme to digest the strongest antibiotic we have, carbapenem, into a harmless waste product. Bacillus anthracis hangs out in permafrost for decades, waiting for warm temperatures. When it's kicked out of human apes, yellow fever virus takes shelter in wild monkeys. Brucella slip inside our cells to avoid detection by antibodies, the seek-and-destroyers of our immune system. Retroviruses slide inside our goddamn genome to hide! Good luck eradicating that with a shotgun.
As I learned about the speed and stealth of our greatest foe, I started to feel like Cersei Lannister facing Daenerys’s dragons. (Game of Thrones, anyone?) Cersei, binary queen that she is, put it like this: “We fight and die, or we submit and die. I know my choice.” Maybe that’s how infectious disease researchers have been looking at our war with microbes. Drug resistance, zoonoses, superbugs, spillovers… it’s a losing battle, but we’d rather die fighting than watching from the sidelines. But what if those aren’t the only two choices?
I suggest that another choice exists, the same one I wrote about last week in Edge Effects: collaborative, multispecies survival, a concept from Anna Tsing.
But does that mean, exactly? I started a list of “solutions” to microbes in my notebook and tried to decide where each one falls on the Collaborative Survival Scale. On the less desirable end of this scale are annihilation of other life forms, human monoculture, and collapse. On the more desirable end are collaboration with other life forms, multispecies ecosystems, and survival.
Antibiotics
Simply put, antibiotics are medicines that kill bacteria. With a name that literally means "against life," these tend toward the annihilation side of the scale, but there are levels of death within antibiotics. I watched a DIERN presentation on veterinary antibiotic use, and learned that the four levels of antibiotic dosing are therapeutic, metaphylactic, prophylactic, and additive.
This slide from DIERN does a good job summing them up. The three arrows, from left to right, indicate "dose," "duration," and "discussion" (meaning controversy). Therapeutic antibiotics have the highest dose, shortest duration, and lowest controversy. Additives have the lowest dose, longest duration, and highest controversy.
Vaccines
Vaccines are medicines that boost our immune systems against specific microbes, such as viruses or bacteria. Instead of killing microbes directly, vaccines help our body's biological microbe-fighting systems (antibodies, T-lymphocytes, B-lymphocytes, macrophages, and others) prepare for war by introducing a small quantity of the pathogen (or, more likely, a dead bit of a pathogen) called an antigen. Our immune system recognizes that bit of the pathogen and produces weapons against it, so if the real pathogen arrives, it won't stand a chance.
Vaccines are held up as one of the best alternatives to antibiotics because microbes can't evolve resistance to them directly. But I started to wonder: could microbes evolve resistance to our own immune system?
The answer is a definite yes. The evolutionary arms-race between pathogens and hosts has been going on since life itself began. HIV is a prime example: so far, the virus has evolved at least fourteen "escape mutations" to evade specific immunity molecules. This game of hide-and-seek has had enormous impacts on the evolutionary path of every host, including humans. It may even explain why we have sexual reproduction.
As I thought about vaccines, I realized they post the same risk of resistance as antibiotics, albeit on a longer time-scale. By boosting the quantity of immune molecules to which pathogens are exposed, vaccines must be increasing the selective pressure on microbes to evade our immune system. I dread the day when a microbe develops resistance not only to our drugs, but to our bodies’ defense. Unlike antibiotic resistance, which can be addressed by the development of new drugs, immune-system resistance cannot be invented away. It would take hundreds of generations and much human suffering to evolve new immune defenses.
The crucial difference between antibiotics and vaccines is that antibiotics are the weapons, while vaccination relies on our immune system to provide the weapons. Although neither is an ideal tool for collaborative survival, vaccines seem to be a solution that will last longer before the bugs outsmart us, if only because our immune systems are more complex and dynamic than the individual chemicals present in antibiotics.
Genetic Improvement
I bring up this solution in the context of livestock, not humans. I consider this tactic a version of "assisted evolution," in which humans amplify selective pressures from pathogens by allowing only disease-resistance individuals to breed. Joel Salatin has long argued for breeding hardy chickens, and programs to improve the genetics of cattle through breeding are widespread.
Evolution through selective pressure is a proven process for living well with microbes. It's the primary tool that host species have used to coexist with microbes for four billion years, and it's dynamic. Theoretically, microbes can't evolve resistance to genetic improvement, because the livestock genes can always keep changing. In this case, we are still engaged in a war with microbes, but we are using evolution to provide the weapons.
Probiotics
Now I am straying into the realm of my own solutions, because I didn't hear mention of this at DIERN. Probiotics come to mind as a way to fight microbes with microbes, to control life with other life. The idea is to consume beneficial bacteria on purpose, most often Lactobacillus and Bifidobacterium. But the current state of affairs is summed up by the National Institute of Health like this: "We still don’t know which probiotics are helpful and which are not." I'm putting probiotics high on the Collaborative Survival scale because they rely on another age-old principle of ecology, biotic competition.
Body-Wide Symbioses (a flourishing microbiome)
Our body is built of more bacterial cells than human ones. Microbes digest our food, eat dust off our eyelashes, and keep our vaginas free from invaders. The most obvious solution to infectious disease seems, to me, to be a cultivated garden of diverse microbes living within and with-on us.
Perhaps garden isn't the right word, because that refers to a group of plants. A zoo comes to mind, but that's for animals. Microzoo? Endo-garden? We call a group of bacteria a culture or a colony, but when we speak of a functional community of microbes living with a body, the term microbiome rings true.
Biome-Wide Symbioses (a flourishing ecosystem)
The more I learned about antibiotic resistance, the more I wondered how non-human organisms deal with pathogens, these apparently unstoppable enemies. Time and again, I ran into examples of symbioses with other species. Salmon rely on cleaner fishes to rid their lice. Cattle egrets and cattle tyrants are two birds who have earned their names from performing the same service for our ubiquitous companions, the cows. Four years ago, when I lived in the Galápagos, I studied a similar interaction between parasite-eating wrasse and green sea turtles.
Now that I think about it, I did hear one example of this idea at DIERN. Brazilian epidemiologists are infecting Aedes aegypti mosquitoes -- the notorious vectors of zika, dengue, and other viruses -- with a bacterium called Wolbachia pipientis. You know what they say: a pathogen of a pathogen is a friend!
To test this idea of biome-wide symbioses as a strategy to control disease, a mad scientist might propose an experiment in which she toppled an existing symbiotic system and then measured the change in health of its organisms. Unfortunately, while this experiment sounds destructive and unethical, it is already being carried out around the world as ecosystems are degraded.
In Brazil, a 50% increase in malaria resulted from a 4% deforestation by area. Here in Madagascar, the September forest-burning season forces black rats to flee toward villages, where their fleas can pass bubonic plague to humans. Ecosystems in distress have the potential to lose the balance mechanisms between hosts and pathogens. As David Quammen puts it in Spillover, "Shake a tree, and things fall out." Perhaps the converse, then, is to cultivate a forest of trees where things stay put.
I came to realize that collaborative survival requires placing our pathogens, and ourselves, back into functioning ecosystems.
Disease has become the major Anthropocene concern for humans and our domestic animals because we have removed ourselves from a functioning, multispecies web. We’ve exponentially increased the resources available to microbes -- cow and human bodies -- while simultaneously removing those resources from their context, the biological interactions that kept pathogens in check.
I hypothesize that humans will be more successful at flourishing on this planet if we reframe our war against pathogens as survival alongside microbes, some of which cause us harm under certain conditions. Sensing and appreciating microbes for themselves is a first step; understanding their ecology is a second; reestablishing functional ecosystems inclusive of us and our livestock is a third.
Cultivating curiosity and compassion for microscopic life sounds like a refreshing and even enjoyable path, far superior to fighting a losing battle just to say we went down fighting. (I'm looking at you, Cersei.)
Do you have that one study trick when you want to get ideas flowing? Maybe you need perfect silence of the library quiet room, or Frank Ocean in your earbuds. Simón Bolívar claimed to do his best thinking at the center of a crowded ballroom. Turns out, the overly-chilled halls of an infectious disease conference were my ideal habitat for incubating ideas.
Idea #1: How Might Our Relationship to Microbes Be Different if We Weren’t So Dang Visual?
Our sight makes us biased. We save colorful species from extinction, yet we wonder if little brown birds can be that important to an ecosystem. We photograph wildflowers and ignore bark, stems, and roots. We cuddle stuffed jaguars and lions, but when was the last time you snuggled a plush microbe? (They do exist!)
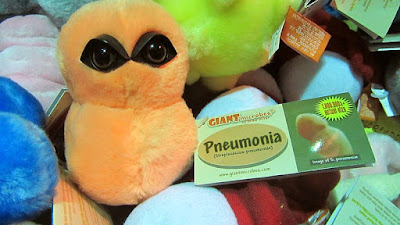 |
| A fluffy Streptococcus pneumoniae so you can finally fulfill your desire to snuggle pneumonia. Photo credit: Wikimedia Commons. |
 |
| An embroidered syphilis sculpture available on the Forgottenland Etsy for $80. |
These two months in Brazil, I have not seen a single microbe. Why? Simple. I don’t have a microscope. Sure, I’ve seen the effects of the single-celled ones: an oozing wound in the back of a dachshund, a syringe full of hot-pink rabies antigen, a can of beer.
 |
| An infected sore on the back of Seo Claudio's dachshund was evidence of bacteria, but I could hardly tell anything about the microbes from this observation. |
But it’s not the same as seeing the organisms themselves. Would you go on a jaguar tour to look at the scratch marks left on a tree? (Ok, jaguar scratches are pretty awesome, but the real thing would be cooler!)
 |
| Scratch marks on the mossy bark of a tree in Bonito. I like to imagine they were left by a jaguar, but the organism itself would leave a much larger impression. |
Our excellent eyesight is limited by scale. We can’t see anything narrower than 0.04 millimeters. At least, we can't distinguish an object smaller than 0.04 millimeters from its neighbor. When we see a conglomeration of tiny particles, like the atoms in a table or the mold cells in a colony, we see their cumulative mass, not their individual bodies. Our eyesight's resolution probably isn't going to get much better, because it's already approaching its quantum limit.
What about our other senses? The linings of our nostrils can differentiate molecular structures of odorants, and our tongues taste the contours of tiny particles, like salt and sugar, with impressive fidelity. But both senses require billions of particles to cross the detection threshold. According to these pretty cool calculations, human taste and smell are operating at 10 orders of magnitude above the quantum limit, meaning that if evolution had taken a different course, we might be a species intimately aware of our single-celled cousins.
 |
| Vanilin |
 |
| Eugenol |
What would our relationship to microbes be like if we were a primarily smelling or tasting organism? Might we know salmonella and leptospira like we do jaguars and lions? Might we develop compassion and curiosity for pathogens, despite their ability to harm us? After all, we find a place in our hearts for macrobes that threaten the same: wolves, pumas, bears, and on down the list of beloved predators.
And that brings me to my next idea.
Idea #2: Writing Microbes Sensually
One of the first things I learned in my favorite college course, Don Snow's “The Nature Essay,” was to write sensually. Breathe in Ellen Meloy's juniper scent, feel Amy Irvine's canyon mud suck your feet down, taste durian through David Quammen's prose. These nature writers push beyond vision to awaken worlds for their readers.
 |
| Write me a story from the perspective of the brain fungus that caused this ant to freeze in its tracks. |
 |
| Show me schistosomiasis, not just the symptoms of a human infection but the sensual details of what it's like to live within the body of a snail. |
Could we write microbes sensually? The genre might be called “speculative biofiction.” I want someone to evoke the satin skin of a gram-negative bacterium, the rigid reluctance of a gram-positive. I want to imagine the sour tang of Yersinia or the sweet tickle of Plasmodium on the tongue. (No sampling pathogens, please!) I want to attend a party of Lactobacillus through scent, following their appetites as they converge on a silo of sprouted barley and nibble in into beer.
 |
| I want to read a poem about this decadent feast, a decomposing cow in a vereda, the endemic wetland of the Cerrado. Which microbes live only in veredas, hoping for cows to die? |
 |
| I want to know the inner workings of a gall wasp larva. How does it trick this leaf to house its invader? |
 |
| How do the algal cells treat their fungal symbionts? What's it like living in a matrix of your neighbor's body? |
By now you might be asking… why does it matter if we have compassion and curiosity for microbes?
Idea #3: We Are Ignorant of Microbes as Individuals, so We Fear Them
Total microbe count: one.
Chikungunya was paired with images of swollen ankles, tuberculosis with scatter plots, candida with symptom charts. I knew I wouldn’t get to smell, taste, or feel microbes at a professional conference, but damn, I barely got to see a picture!
 |
| The only microbe actually shown all day was this yellow fever virion. I was so excited, I sketched yellow fever for the next half hour and forgot to listen... whoops! |
We don't know our microbes. That ignorance contributes to our fear. And, sometimes, that fear leads us to overreaching and violent reactions to microbes.
And I think our skewed perception, our tendency to ignore the subvisible, might be confounding our imagination when it comes to living well with microbes. I listened to researchers who seek “solutions” to the “problem” of disease. I also heard, over and over, our failure to find that solution.
 |
| A perfect illustration of our one-dimensional relationship with microbes based on fear. This slide is from a DIERN presentation I watched on antibiotic resistance. |
 |
| This campaign to eradicate leishmaniasis paints the bacterium's vector, the sand fly, like a dangerous and wanted criminal. |
And I think our skewed perception, our tendency to ignore the subvisible, might be confounding our imagination when it comes to living well with microbes. I listened to researchers who seek “solutions” to the “problem” of disease. I also heard, over and over, our failure to find that solution.
“Aedes aegypti mosquito vector eradicated in Brazil! Accidentally reintroduced twice…”
“Antibiotic kills Mycobacterium tuberculosis! Now, multi-resistant Tb is more lethal than ever…”
“Yellow fever was conquered for good! Now it's reemerging as climate shifts the habitat of its wildlife host, Amazonian monkeys….”
 |
| The multiple "eliminations" followed by "reinfestations" of the Aedes aegypti mosquito make eradication seem like a less-than-permanent state. |
 |
| This slide depicts four drivers of yellow fever re-emergence in Brazil. The "R" in DIERN stands for re-emerging diseases, a sign that annihilation of microbial enemies may be a dead-end tactic. |
The story of disease I heard at the DIERN conference tells that humans are engaged in warfare with microbes. We grasp onto this narrative because it's familiar. We have been waging war on macro-predators for millennia, and we've been winning. Saber-toothed lions went extinct; gray wolves and Bengal tigers are confined, for the most park, to controlled populations in parks. Although predators still take lives (read about human-wildlife conflict in Nepal, California, or Brazil), their impact on the human species is a shadow of what it once was.
But I think this narrative of war makes less sense when we look at our relationship with microbes. Our campaigns against large predators worked because we share a scale. Our smaller foes, the microbes, will not be so easy to knock off. If we declare war, we may be setting ourselves up to lose.
Idea #4: We Are Not Going to Win This War
Speed, in terms of evolution. Microorganisms evolve faster than you can load a YouTube video on sketchy WiFi. The typical generation time of E. coli is 20 minutes. The average for a human is about 15,000,000 minutes. Shorter generations allow faster evolution. E. coli and their ilk have us beat with their hands (ahem, flagella) tied.
Stealth, in terms of hiding from us. Tiny things are not only hard to see with our eyes, they are also hard to detect and target with our weapons, like medicines and immune systems. They evade our weapons by evolving around them. In the last eight years, Enterobacteria have started producing an enzyme to digest the strongest antibiotic we have, carbapenem, into a harmless waste product. Bacillus anthracis hangs out in permafrost for decades, waiting for warm temperatures. When it's kicked out of human apes, yellow fever virus takes shelter in wild monkeys. Brucella slip inside our cells to avoid detection by antibodies, the seek-and-destroyers of our immune system. Retroviruses slide inside our goddamn genome to hide! Good luck eradicating that with a shotgun.
 |
| A playbook for the war against microbes, "Tackling Antimicrobial Resistance on Ten Fronts," published by the Review on Antimicrobial Resistance and featured in one of the presentation I watched. |
Idea #5: Curiosity and Compassion as a Foundation for Collaborative Survival with Microbes
I suggest that another choice exists, the same one I wrote about last week in Edge Effects: collaborative, multispecies survival, a concept from Anna Tsing.
But does that mean, exactly? I started a list of “solutions” to microbes in my notebook and tried to decide where each one falls on the Collaborative Survival Scale. On the less desirable end of this scale are annihilation of other life forms, human monoculture, and collapse. On the more desirable end are collaboration with other life forms, multispecies ecosystems, and survival.
Antibiotics
Simply put, antibiotics are medicines that kill bacteria. With a name that literally means "against life," these tend toward the annihilation side of the scale, but there are levels of death within antibiotics. I watched a DIERN presentation on veterinary antibiotic use, and learned that the four levels of antibiotic dosing are therapeutic, metaphylactic, prophylactic, and additive.
- Therapeutic antibiotics are given to a sick, diagnosed, individual animal at a high dose for a short duration of time. (This is probably how you have experienced antibiotics prescribed by your doctor.) This usage poses little risk of developing antibiotic resistance because all the bacteria are killed, and the exposure of microbes to the medicine is limited.
- Metaphylaxis is when antibiotics are given to a herd of animals, a few of which are showing clinical symptoms of disease.
- Prophylaxis is a preventative measure, when antibiotics are given to a group of animals that are not showing clinical symptoms, but may be at risk for disease.
- Additive antibiotics are those given indefinitely to all animals on a property, at low dosage, to promote faster growth and lower production costs. This usage poses a high risk of developing resistance, because only the weakest bacteria are killed, and there is prolonged selective pressure on microbes to evolve defenses to the medicine.
 |
| A version of my Collaborative Survival Scale for veterinary antibiotics. |
In conclusion, additive antibiotics are tools of unilateral collapse, whereas therapeutic antibiotics have an important, but limited, role to play in health. Overall, antibiotics are a weapon, better suited to wars than to collaborative survival.
Vaccines are medicines that boost our immune systems against specific microbes, such as viruses or bacteria. Instead of killing microbes directly, vaccines help our body's biological microbe-fighting systems (antibodies, T-lymphocytes, B-lymphocytes, macrophages, and others) prepare for war by introducing a small quantity of the pathogen (or, more likely, a dead bit of a pathogen) called an antigen. Our immune system recognizes that bit of the pathogen and produces weapons against it, so if the real pathogen arrives, it won't stand a chance.
 |
| Here, I'm vaccinating a cat in my host-town of Taboco. It's easy when you hold the cat against a tree or post, because it grabs on with its claws and holds still. |
Vaccines are held up as one of the best alternatives to antibiotics because microbes can't evolve resistance to them directly. But I started to wonder: could microbes evolve resistance to our own immune system?
The answer is a definite yes. The evolutionary arms-race between pathogens and hosts has been going on since life itself began. HIV is a prime example: so far, the virus has evolved at least fourteen "escape mutations" to evade specific immunity molecules. This game of hide-and-seek has had enormous impacts on the evolutionary path of every host, including humans. It may even explain why we have sexual reproduction.
As I thought about vaccines, I realized they post the same risk of resistance as antibiotics, albeit on a longer time-scale. By boosting the quantity of immune molecules to which pathogens are exposed, vaccines must be increasing the selective pressure on microbes to evade our immune system. I dread the day when a microbe develops resistance not only to our drugs, but to our bodies’ defense. Unlike antibiotic resistance, which can be addressed by the development of new drugs, immune-system resistance cannot be invented away. It would take hundreds of generations and much human suffering to evolve new immune defenses.
The crucial difference between antibiotics and vaccines is that antibiotics are the weapons, while vaccination relies on our immune system to provide the weapons. Although neither is an ideal tool for collaborative survival, vaccines seem to be a solution that will last longer before the bugs outsmart us, if only because our immune systems are more complex and dynamic than the individual chemicals present in antibiotics.
Genetic Improvement
I bring up this solution in the context of livestock, not humans. I consider this tactic a version of "assisted evolution," in which humans amplify selective pressures from pathogens by allowing only disease-resistance individuals to breed. Joel Salatin has long argued for breeding hardy chickens, and programs to improve the genetics of cattle through breeding are widespread.
 |
| Ted Turner's Flying D Ranch in Montana uses American bison, Bison bison, to produce burgers from a native, disease-resistant species. Collaborative Survival Ranking: high. |
Probiotics
Now I am straying into the realm of my own solutions, because I didn't hear mention of this at DIERN. Probiotics come to mind as a way to fight microbes with microbes, to control life with other life. The idea is to consume beneficial bacteria on purpose, most often Lactobacillus and Bifidobacterium. But the current state of affairs is summed up by the National Institute of Health like this: "We still don’t know which probiotics are helpful and which are not." I'm putting probiotics high on the Collaborative Survival scale because they rely on another age-old principle of ecology, biotic competition.
Body-Wide Symbioses (a flourishing microbiome)
Our body is built of more bacterial cells than human ones. Microbes digest our food, eat dust off our eyelashes, and keep our vaginas free from invaders. The most obvious solution to infectious disease seems, to me, to be a cultivated garden of diverse microbes living within and with-on us.
Perhaps garden isn't the right word, because that refers to a group of plants. A zoo comes to mind, but that's for animals. Microzoo? Endo-garden? We call a group of bacteria a culture or a colony, but when we speak of a functional community of microbes living with a body, the term microbiome rings true.
Biome-Wide Symbioses (a flourishing ecosystem)
The more I learned about antibiotic resistance, the more I wondered how non-human organisms deal with pathogens, these apparently unstoppable enemies. Time and again, I ran into examples of symbioses with other species. Salmon rely on cleaner fishes to rid their lice. Cattle egrets and cattle tyrants are two birds who have earned their names from performing the same service for our ubiquitous companions, the cows. Four years ago, when I lived in the Galápagos, I studied a similar interaction between parasite-eating wrasse and green sea turtles.
 |
| A cattle tyrant surfs the head of a capybara, world's largest rodent and a host for disease-carrying Amblyomma ticks. |
 |
| A green sea turtle is grazed by white salema (Xenichthys agassizii) off San Cristóbal, a Galápagos Island. |
 |
| Some people in the United States keep guinea fowl for their tick-hunting reputation, but everyone I spoke with in Brazil insisted the spherical hens were only around to look pretty. |
To test this idea of biome-wide symbioses as a strategy to control disease, a mad scientist might propose an experiment in which she toppled an existing symbiotic system and then measured the change in health of its organisms. Unfortunately, while this experiment sounds destructive and unethical, it is already being carried out around the world as ecosystems are degraded.
 |
| Rolling cattle pasture in Brazil where Cerrado forest previously harbored a complex web of plants, animals, and microbes. |
Idea #6: Placing Ourselves Into Ecosystems
I came to realize that collaborative survival requires placing our pathogens, and ourselves, back into functioning ecosystems.
Disease has become the major Anthropocene concern for humans and our domestic animals because we have removed ourselves from a functioning, multispecies web. We’ve exponentially increased the resources available to microbes -- cow and human bodies -- while simultaneously removing those resources from their context, the biological interactions that kept pathogens in check.
I hypothesize that humans will be more successful at flourishing on this planet if we reframe our war against pathogens as survival alongside microbes, some of which cause us harm under certain conditions. Sensing and appreciating microbes for themselves is a first step; understanding their ecology is a second; reestablishing functional ecosystems inclusive of us and our livestock is a third.
Cultivating curiosity and compassion for microscopic life sounds like a refreshing and even enjoyable path, far superior to fighting a losing battle just to say we went down fighting. (I'm looking at you, Cersei.)
 |
| (Psst! You forgot collaborative survival!) |










